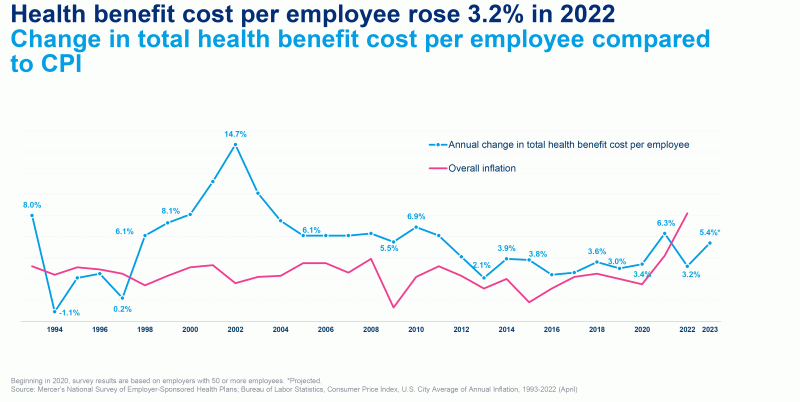
Health benefits costs rose by 3.2% this year, and employers are bracing for an even larger hike in 2023, a new survey shows.
Analysts at Mercer polled more than 2,000 employers representing 124 million full-time and part-time employees and found that they expect benefits costs to increase by 5.4% next year. And they're expecting faster cost growth to continue in the near future, according to the survey.
Cost growth spiked in 2021 to 6.3% as more people sought out care delayed by COVID-19. This year's rate of 3.2% may seem like a return to normalcy after an errant year in 2021, but the analysts warned that healthcare cost rates typically grow faster than inflation, which this year was 8%.
“In the healthcare sector, higher wages, labor shortages, and consolidation will almost certainly result in higher prices,” Sunit Patel, chief health actuary at Mercer, said in the release.
“One reason cost growth lagged inflation this year is because healthcare providers typically have multi-year contracts with health plans," Patel said. "So although employers did not feel the full brunt of inflation immediately, it’s very likely that inflation-driven cost increases will phase in over the next few years as contracts are renewed.”
Total health benefit costs per employee reached $15,013 on average in 2022, with small businesses with between 40 and 499 workers reporting slightly higher costs compared to their larger counterparts.
Large employers typically offer more extensive benefits but can self-fund their plans, allowing them to save on risk charges from the insurance company. Larger firms also have more resources to put toward health program management, Mercer said.
As costs rise, employers are facing a tight labor market that they're making a priority, according to the survey. Before the pandemic, cost-management strategies were a top focus for these companies, previous Mercer surveys show, but this year "enhancing benefits to improve attraction and retention" was at the top, cited as very important or important by 84% of those surveyed.
About three-quarters (73%) said adding programs or services to improve access to behavioral health care was important, and 68% said the same about affordability.
In a complex financial environment, employers are still aiming to avoid cost-shifting to employees as they weigh strategies to address affordability, the survey found. Employers are also hesitant to offer just a high-deductible health plan to members, particularly very large employers with 20,000 or more employees.
How are employers managing cost increases while minimizing cost-shifting? The survey found that a third of large employers (35%) and half of very large employers (53%) are focusing on high-performance networks and high-value care.
Thirty-six percent of very large employers said they offer telephonic services to assist with navigation, and 17% offer digital tools.
“The affordability issue cuts both ways. Employers will be challenged to absorb the higher costs coming down the pike, but they also know some people will forego important care when they feel they can’t afford it,” said Tracy Watts, national leader for U.S. health policy at Mercer, in the release. “Particularly with inflation putting added stress on household finances, budget concerns need to be balanced with the downstream implications of healthcare affordability. So the focus now is on strategies to rein in cost growth without shifting the cost to the employee.”