Planned mergers between major health companies could lead to a serious anticompetitive landscape, a new analysis finds.
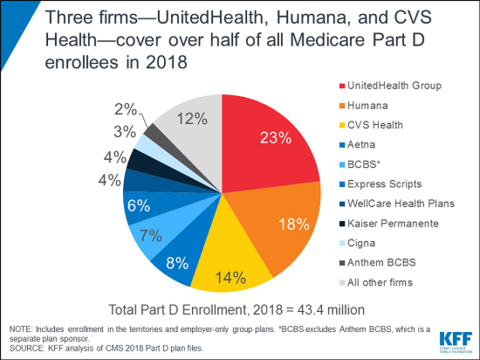
The proposed mergers of Cigna-Express Scripts and CVS Health-Aetna would further consolidate the Medicare Part D marketplace, research by the Kaiser Family Foundation found. The merged entities, plus Humana and UnitedHealth, would cover 71% of all Part D beneficiaries.
That type of dominance in the Part D market is comparable to Verizon and AT&T's command of the wireless carrier industry. Those two companies occupy about 69% of the market, according to Statista.
RELATED: Health insurance CEOs earned $342.6M in 2017
Currently, three companies—UnitedHealth, Humana and CVS—already account for more than half of the program's 43 million beneficiaries.
Critics of the mergers, including the American Medical Association, have said the deals, particularly CVS-Aetna, pose anticompetitive concerns, "unique to vertical mergers," as new competitors would have to enter the market in both insurance and PBM to compete with the combined CVS-Aetna.
We continue "to strongly encourage state and federal officials to rigorously review the proposed mergers between pharmacy benefit managers and health insurers given the potential negative impact on pharmaceutical benefit management services, local health insurance markets, as well as local retail pharmacy markets, which in turn can harm consumers in these markets," David O. Barbe, president of AMA, told FierceHealthcare in an email. "Close scrutiny is needed to determine if the ramifications of these massive mergers will threaten the benefits of competition, including increased access and choice, lower prices and higher quality care for patients.”
The companies, however, have argued that the deals will allow for more integrated care and will increase competition in the PBM sector, and lower drug costs for patients.
The Trump administration is pushing for more competition in the Part D market as part of a drug pricing blueprint, seemingly putting the mergers at odds with the White House's vision.
RELATED: Trump targets Medicare, PBMs in plan to lower drug prices
The Department of Justice is currently reviewing the $69 billion deal between CVS and Aetna and has given few clues on whether the transaction will be approved. With its business-friendly approach, one might expect the White House to be more open to such a deal than the Obama administration, which blocked the Anthem-Cigna and Aetna-Humana deals.
However, the Trump administration's decision to block the AT&T-Time Warner deal could indicate the proposed healthcare mergers might ultimately be too big, and too anticompetitive, to approve.